|


|
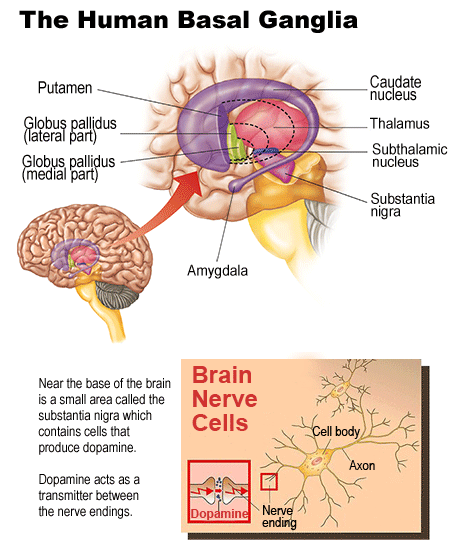
 There are hundreds of articles parroting each other on the internet talking about what causes Restless Legs Syndrome. The two most agreed upon theories are an imbalance of dopamine (a chemical that transmits signals between nerve cells in the brain) and low iron levels. I'm going to present evidence that both of these conditions could be caused by the presence of inflammation. In other words, I believe inflammation to be the primary condition while restless legs, dopamine imbalance and low irons levels are simply effects of this chronic state. Because of the dopamine theory, hundreds of millions of dollars worth of horrendous dopamine agonist drugs (drugs with terrible side-effects that were created for Parkinson's patients) have been blindly dished out by doctors to their RLS patients. This page provides scientific evidence that inflammation can affect dopamine levels. For information on how inflammation can affect iron levels, please visit the page Scientific Studies Showing How Inflammation Can Affect Iron Levels . 
Mild elevations in Dopamine are associated with addictions. Nicotine, cocaine, and other substances produce a feeling of excited euphoria by increasing Dopamine levels in the brain. Too much of these chemicals/substances and we feel "wired" as moderate levels of Dopamine make us hyperstimulated - paying too much attention to our environment due to being overstimulated and unable to separate what's important and what is not. In an ADHD child, low levels of Dopamine don't allow the child to focus or attend to anything in the environment, looking very physically hyperactive when running about the room or switching from activity-to-activity due to their lack of focus. As Dopamine levels increase above the normal range, our ability to focus increases to the point of being paranoid. Mild elevations make the environment overly stimulating and excited. Joseph M. Carver, Ph.D. "Dopamine: Parkinson's Disease and ADHD to Smoking and Paranoia" eNotAlone.com www.enotalone.com/article/4115.html  Most research on the disease mechanism of Restless Legs Syndrome has focused on the dopamine and iron system. These hypotheses are based on the observation that iron and levodopa can be used to treat RLS, levodopa being a medicine for treating hypodopaminergic (low dopamine) conditions, and also on findings from functional brain imaging (such as positron emission tomography and functional magnetic resonance imaging), autopsy series and animal experiments. R. Allen, "Dopamine and iron in the pathophysiology of restless legs syndrome (RLS)". Sleep Med. 5 (4): 385-91. (July 2004) doi:10.1016/j.sleep.2004.01.012. PMID 15222997. S. Clemens, D. Rye and S. Hochman "Restless legs syndrome: revisiting the Dopamine hypothesis from the spinal cord perspective". Neurology 67 (1): 125-130. (2006). doi:10.1212/01.wnl.0000223316.53428.c9. PMID 16832090. www.neurology.org/cgi/content/abstract/67/1/125. CJ Earley, P Barker, A. Horska and RP Allen, "MRI-determined regional brain iron concentrations in early- and late-onset restless legs syndrome". Sleep Med. 7 (5): 458-61. (August 2006). doi:10.1016/j.sleep.2005.11.009. PMID 16740411  A dopamine agonist is a compound that activates dopamine receptors in the absence of dopamine. Dopamine agonists activate signaling pathways through the dopamine receptor and trimeric G-proteins, ultimately leading to changes in gene transcription. Some medical drugs act as dopamine agonists and can treat hypodopaminergic (low dopamine) conditions; they are typically used for treating Parkinson's disease and certain pituitary tumors (prolactinoma), and may be useful for restless legs syndrome (RLS). Both Requip (Ropinirole) and Mirapex (Pramipexole) are FDA-approved for the treatment of RLS. "Dopamine Agonist" WikiPedia en.wikipedia.org/wiki/Dopamine_agonist Its mechanism of action is to work on dopamine receptors so that they are stimulated. This is different than adding dopamine to the body, which would stimulate the receptors, and it's also distinct from preventing the body from taking up (reuptake) free dopamine so there is more in use. Instead, it's something like a substitute for dopamine that can fool dopamine receptors into working, even when the body lacks a good supply of this neurotransmitter. Tricia Ellis-Christensen, "What Is a Dopamine Agonist?" wiseGEEK www.wisegeek.com/what-is-a-dopamine-agonist.htm  Some of the common side effects of dopamine agonists include: * Euphoria * Hallucinations * Causing or worsening psychosis * Orthostatic hypotension * Increased orgasmic intensity * Weight loss * Nausea * Insomnia * Unusual tiredness or weakness * Dizziness, drowsiness, lightheadedness, or fainting * Twitching, twisting, or other unusual body movements * Pathological addiction (gambling, shopping, internet pornography, hyper-sexuality) "Dopamine Agonist" WikiPedia en.wikipedia.org/wiki/Dopamine_agonist  "Why dopamine neurons are especially vulnerable to this inflammatory insult is still unknown. Dr. Glass noted that astrocytes and microglia are more concentrated in the substantia nigra than in other parts of the brain - it could just be a concentration effect, he said. It's also possible that dopamine neurons are more sensitive to whatever toxic factors are produced. The culprit toxic molecules are still unknown, but there are plenty of candidates, including cytokines, death pathway triggers, and others. It's a complicated problem to sort out." Richard Robinson, "To Protect Dopamine Neurons, Turn on Nurr1, Turn Off Inflammation." Neurology Today: 21 May 2011 - Volume 9 - Issue 10 - pp 21,23. doi: 10.1097/01.NT.0000354539.50613.77 "Evidence suggests that chronic inflammation, mitochondrial dysfunction, and oxidative stress play significant and perhaps synergistic roles in Parkinson's disease (PD), where the primary pathology is significant loss of the dopaminergic neurons in the substantia nigra." RL Hunter, N. Dragicevic, K. Seifert, DY Choi, M. Liu. HC Kim, WA Cass, PG Sullivan and G. Bing, "Inflammation induces mitochondrial dysfunction and dopaminergic neurodegeneration in the nigrostriatal system." Journal of Neurochemistry. 2007 Mar;100(5):1375-86. Epub 2007 Jan 23.PMID: 17254027 "We tested the effects of inflammation on renal dopamine D1 receptor signaling cascade, a key pathway that maintains sodium homeostasis and blood pressure during increased salt intake. Inflammation was produced by administering lipopolysaccharide (LPS; 4 mg/kg ip) to rats provided without (normal salt) and with 1% NaCl in drinking water for 2 wk (high salt). Our results suggest that LPS differentially regulates NF-kappaB and Nrf2, produces inflammation, decreases antioxidant enzyme, increases oxidative stress, and causes D1 receptor dysfunction in the RPTs. The LPS-induced dysfunction of renal D1 receptors (dopamine receptor) alters salt handling and causes hypertension in rats during salt overload." M. Asghar, G. Chugh and MF Lokhandwala, "Inflammation compromises renal dopamine D1 receptor function in rats." Am J Physiol Renal Physiol. 2011 Dec;297(6):F1543-9. Epub 2011 Sep 30. PMID: 19794106 "Children with ADD have a much higher Silent Inflammation Profile than normal children. Therefore, the problem of ADD is much more complicated than simply the lack of dopamine in the brain." Barry Sears, Ph.D., "Brain Drain Due to Silent Inflammation: ADD to Alzheimer's Disease" The American Chiropractor (May 2006). "Alterations in dopamine receptor function have been reported in human and rodent hypertension. Essential hypertension is associated with dopamine D2 receptor (D2R) gene polymorphisms that result in reduced D2R density. Mice with disruption of the D2R (D2-/) have elevated blood pressure. The D2Rs regulate the inflammatory reaction and are implicated in the pathogenesis of inflammatory diseases. We hypothesized that deficient D2R function increases the expression of pro-inflammatory cytokines and chemokines in the kidney and results in renal inflammation and injury that contribute to the development of high blood pressure. Our results show that the D2R, by mechanisms other than increased oxidant activity, regulates the expression of inflammatory factors in the kidney and suggest that altered D2R function may result in renal inflammation and injury." Ines Armando, Annabelle M. Pascua, Xiaoyan Wang, Yanrong Zhang, Van Anthony, M. Villar, Yu Yang, John E. Jones, Laureano Asico, Crisanto Escano and Pedro A. Jose, "Deficient Dopamine D2 Receptor Function Results in Renal Inflammation and Injury." Children's Rsch Institute- Children's National Med Cntr, Washington, DC. (Circulation. 2011;120:S1165.) "Several lines of evidence point to a significant role of neuroinflammation in Parkinson's disease (PD) and other neurodegenerative disorders." Rosario Sanchez-Pernaute, Andrew Ferree, Oliver Cooper, Meixiang Yu, Anna-Liisa Brownell and Ole Isacson. "Selective COX-2 inhibition prevents progressive dopamine neuron degeneration in a rat model of Parkinson's disease." Journal of Neuroinflammation (2004). 1:6doi:10.1186/1742-2094-1-6 "A massive degeneration of dopamine-containing neurons in the substantia nigra (SN) in the midbrain is characteristic of Parkinson's disease. Inflammation in the brain has long been speculated to play a role in the pathogenesis of this neurological disorder." Bin Liu, Jian-Wei Jiang, Belinda C. Wilson, Lina Du, San-Nan Yang, Jiz-Yuh Wang, Gen-Cheng Wu, Xiao-Ding Cao and Jau-Shyong Hong, "Systemic Infusion of Naloxone Reduces Degeneration of Rat Substantia Nigral Dopaminergic Neurons Induced by Intranigral Injection of Lipopolysaccharide" The Journal of Pharmcology and Experimental Therapeutics Vol. 295, No. 1, JPET 295:125-132, (2000). 
VITAMINS AND SUPPLEMENTS omega 3 "In an omega-3 deficiency, the release of dopamine from the vesicular storage pool under tyramine stimulation is 90-percent lower than in rats receiving an adequate omega-3 intake." Alan C. Logan "Neurobehavioral aspects of omega-3 fatty acids: possible mechanisms and therapeutic value in major depression". Alternative Medicine Review. FindArticles.com. 01 May, 2011. findarticles.com/p/articles/mi_m0FDN/is_4_8/ai_111303983 "A study examining whether omega-3 exerts neuroprotective action in Parkinson's disease found that it did, using an experimental model, exhibit a protective effect (much like it did for Alzheimer's disease as well). The scientists exposed mice to either a control or a high omega-3 diet from two to twelve months of age and then treated them with a neurotoxin commonly used as an experimental model for Parkinson's. The scientists found that high doses of omega-3 given to the experimental group completely prevented the neurotoxin-induced decrease of dopamine that ordinarily occurs. Since Parkinson's is a disease caused by disruption of the dopamine system, this protective effect exhibited could show promise for future research in the prevention of Parkinson's disease." "Omega 3-Fatty Acid." WikiPedia en.wikipedia.org/wiki/Omega-3_fatty_acid M. Bousquet, M. Saint-Pierre, C. Julien, N. Salem, F. Cicchetti and F. Calon, "Beneficial effects of dietary omega-3 polyunsaturated fatty acid on toxin-induced neuronal degeneration in an animal model of Parkinson's disease". Fed Am Soc Exper Bio J 22 (4): 1213???1225. (April 2011). "French scientists have shown that rats deficient in omega-3 fatty acids had more receptors for the neurotransmitter serotonin and a corresponding decrease in dopamine in the frontal cortex. The direction of the changes in these neurotransmitter systems is consistent with some human models of major depression. Not surprisingly, other scientists have observed that increasing the dietary intake of omega-3 fatty acids boosted the levels of the neurotransmitter dopamine in the frontal cortex of rats. In humans, increased dopamine in the frontal cortex increases drive and motivation, attributes lacking in the depressed person." Andrew Stoll, MD, "The Omega-3 Connection: The Groundbreaking Antidepression Diet and Brain Program." Free Press (March 5, 2002) page 117. vitamin b3 (niacin) "Several findings have established the interaction between Serotonin, which is facilitated by Niacin, and Dopamine, a neurotransmitter lacking in patients with ADHD. The findings state that the serotonin system inhibits dopaminergic function at the level of the origin of the dopamine system in the midbrain as well as at the terminal dopaminergic fields in the forebrain. The above findings have led to the speculation that Niacin may treat ADHD." "Niacin And ADHD" scumdoctor.com (2006) www.scumdoctor.com/medicine/vitamin-supplements/vitamin-b3/Niacin-And-Adhd.html "Phenylalanine is the precursor of the amino acid tyrosine, which cannot be reconverted, so phenylalanine is essential in the diet. As a precursor of tyrosine, phenylalanine can form norepinephrine in the brain in addition to other catecholamines such as epinephrine, dopamine, and tyramine. Norepinephrine is an important neurotransmitter (that is, it conveys chemoelectric information at nerve synapses) and is apparently important for memory, alertness, and learning. Phenylalanine metabolism requires pyridoxine (B6), niacin (B3), vitamin C, copper, and iron." Elson M. Haas M.D. "Phenylalanine." Staying Healthy with Nutrition: The Complete Guide to Diet and Nutritional Medicine, Celestial Arts, Berkeley, CA (2006). "A patient with Parkinson's disease taking levodopa/carbidopa, selegiline, buproprion, aspirin and niacin had decreased rigidity and bradykinesia when his niacin dose was steadily escalated for treatment of high triglycerides, but ultimately the patient could not tolerate niacin because of severe nightmares and skin rash. If further research can reproduce this patient's initial beneficial experience while avoiding the adverse effects, niacin could be a useful adjunctive agent for Parkinson's disease, either population-wide or in a pharmacogenomically defined set of responders." Joseph Martin Alisky, "Niacin improved rigidity and bradykinesia in a Parkinson's disease patient but also caused unacceptable nightmares and skin rash???A case report." Journal Nutritional Neuroscience, Volume 8, Issue 5 & 6 October 2005 , pages 327 - 329 DOI: 10.1080/10284150500484638 vitamin b6 "In summary, the present in vivo electrochemical study demonstrated that vitamin B-6 deficiency altered the response of dopaminergic neurons in the striatum. Vitamin B-6-deficient rats had an increased rise time of dopamine release and a longer decay time for the released dopamine to return to the baseline level." Fu-In Tang and Ien-Lan Wei , "Vitamin B-6 Deficiency Prolongs the Time Course of Evoked Dopamine Release from Rat Striatum." 2004 The American Society for Nutritional Sciences J. Nutr. 134:3350-3354 (December 2004). "The impact Vitamin B6 may have on positive levels of neurotransmitters, especially dopamine and epinephrine, should not be overlooked as all performance originates in the mind. Most athletes can benefit from increased focus and intensity." "Vitamin B6: Essential Micronutrient" Nutritional Supplements Knowledgebase www.nutros.com/nsr-0202c.html "Vitamin B6 (pyridoxine) aids in the processing of amino acids, which are the building blocks of all proteins and some hormones. It is needed in the manufacture of serotonin, melatonin and dopamine." Nancy Schimelpfening "Vitamin for Depression? A Good Vitamin Supplement Could Be Just What the Doctor Ordered." About.com Guide (May 04, 2011) depression.about.com/cs/diet/a/vitamin.htm vitamin b11 (folic acid) "The scientists found that mice with low amounts of dietary folic acid had elevated levels of homocysteine in the blood and brain. They suspect that increased levels of homocysteine in the brain caused damage to the DNA of nerve cells in the substantia nigra, an important brain structure that produces dopamine. Loss of dopamine causes the nerve cells to dysfunction, leaving patients unable to direct or control their movement in a normal manner." "Folic Acid Deficiency May Increase Susceptibility to Parkinson's Disease." Alzheimer's Disease Education and Referral Center of the National Institute on Aging (January 14, 2002). www.nia.nih.gov/Alzheimers/ResearchInformation/NewsReleases/Archives/PR2002/PR20020114folicacidparkinsons.htm W. Duan, B. Ladenheim, RG Cutler, II Kruman, JL Cadet and MP Mattson, "Dietary folate deficiency and elevated homocysteine levels endanger dopaminergic neurons." J Neurochem (2002) 80: 101-10. "Folic Acid is a necessary cofactor to the enzyme, tyrosine hydroxylase, which converts tyrosine to L-dopa. Folic acid also serves as a methyl donor in a number of neurotransmitter pathways, including the conversion of norepinephrine to epinephrine." "Glossary of Ingredients." NeuroScience, Inc. www.neurorelief.com/index.php?option=com_content&task=view&id=158&Itemid=48 "According to the American Journal of Psychiatry, taking vitamin supplements can also help increase dopamine levels. Include vitamin B12, folic acid (vitamin B9), omega-3 fatty acids and vitamin B6 in your supplements. The American Journal of Psychiatry in 1997 published a study titled "Folate, Vitamin B12 and Homocysteine in Major Depressive Disorder," which showed that deficiencies in these vitamins are common in those who are depressed." eHow Contributing Writer, "What Is the Best Way to Boost Dopamine in the Brain?" eHow.com www.ehow.com/way_5769612_way-boost-dopamine-brain_.html "The B vitamin thiamine and folic acid increase dopamine levels in the brain." Michael Smith, MD, "Low Libido - It's All in Your Head!" ezinearticles.com ezinearticles.com/?Low-Libido--Its-All-in-Your-Head!&id=2480703 vitamin b12 "High homocysteine levels are common in Parkinson's patients. The use of levodopa treatment in Parkinson's patients further depletes vitamin B12 and folic acid, two vitamins known to reduce homocysteine levels. Increased homocysteine levels accelerate dopaminergic cell death (dopamine-producing cells) in Parkinson's patients through neurotoxic effects." Herrmann, W., Lorenzi, S., Obeid, R. "Review of the role of hyperhomocysteinemia and B-vitamin deficiency in neurological and psychiatric disorders-current evidence and preliminary recommendations." Fortschr Neurol Psychiatr. 2007 Sep; 75 (9): 515-27. Quershi, GA., Quershi, AA., Devrajani, BR, Chippa, MA., Syed, SA. "Is the deficiency of vitamin B12 related to oxidatives stress and neurotoxicity in Parkinon's patients?" CNS Neurol Disord Drug Targets. 2011 Feb;7(1):20-7. "Conversion of tyrosine to l-dopa requires the tyrosine hydroxylase enzyme, which is iron dependent. If the ferritin iron storage protein level is below 50 mcg/L, dopamine production can be decreased and restless leg syndrome can occur. Folic acid megadoses of 5,000 micrograms, sublingual Vitamin B12, Vitamin B12 subcutaneous injections or ferrous bisglycinate supplements can usually increase ferritin levels above 50 mcg/L." Steven Sponaugle, "Nonpsychostimulant Dopamine Enhancement for Attention Deficit Disorder Treatment." (June 9, 2011). Stevensponaugle's Blog stevensponaugle.wordpress.com/2011/07/09/nonpsychostimulant-dopamine-enhancement-for-attention-deficit-disorder-treatment "Several recent studies indicate a relationship between B12, homocysteine, and Alzheimer's. B12 status is routinely measured at the time of Alzheimer's diagnosis, and there is some indication that ongoing measurements may be useful to detect the development of a severe deficiency. Siuda J, Gorzkowska A, Patalong-Ogiewa M, et al. (2011). "From mild cognitive impairment to Alzheimer's disease - influence of homocysteine, vitamin B12 and folate on cognition over time: results from one-year follow-up". Neurologia I Neurochirurgia Polska 43 (4): 321-9. PMID 19742390. http://www.neurology.termedia.pl/showarticle.php?id=13058. Kivipelto M, Annerbo S, Hultdin J, et al. (July 2011). "Homocysteine and holo-transcobalamin and the risk of dementia and Alzheimers disease: a prospective study". European Journal of Neurology 16 (7): 808-13. doi:10.1111/j.1468-1331.2011.02590.x. PMID 19453410. Kageyama M, Hiraoka M, Kagawa Y (October 2011). "Relationship between genetic polymorphism, serum folate and homocysteine in Alzheimer's disease" ([dead link]). Asia-Pacific Journal of Public Health 20 Suppl: 111-7. PMID 19533869. http://aph.sagepub.com/cgi/pmidlookup?view=long&pmid=19533869. Prodan CI, Cowan LD, Stoner JA, Ross ED (September 2011). "Cumulative incidence of vitamin B12 deficiency in patients with Alzheimer disease". Journal of the Neurological Sciences 284 (1-2): 144-8. doi:10.1016/j.jns.2011.05.005. PMID 19464701 vitamin c (ascorbic acid) "Vitamin C is important and necessary for the synthesis of the neurotransmitters, norepinephrine and serotonin. It catalyzes the conversion of dopamine to norepinephrine and the conversion of tryptophan to serotonin." "Vitamin C - Ascorbic Acid" Springboard (2004). www.springboard4health.com/notebook/v_c.html "Vitamin C is also a part of the production of dopamine, noradrenalin and adrenaline in the nervous system. Dopamine is critical for the brain's ability to control movement and a lack of dopamine will give symptoms similar to those shown in Parkinson's disease. It's the chemical that helps us to experience pleasure. Whenever we do something good, like eating, the brain will release a little dopamine into the body as a form of positive reinforcement. A lack of it is thought to play a role in many neurological disorders." Vincent Platania, "Benefits of Vitamin C" Buzzle.com www.buzzle.com/articles/benefits-vitaminc-body-collagen-diet.html "Each of the primary neurotransmitters has a nutrient precursor, and dopamine is derived from the amino acids phenylalanine and tyrosine. Co-factors such as folic acid, vitamin B6, iron, copper and vitamin C are important for phenylanaline to be absorbed and utilized." "Dopamine." Caring Medical & Rehabilitation Services, Oak Park, IL www.caringmedical.com/media/article.asp?article_id=520 vitamin e "Vitamin E showed a protective effect against PCB-induced toxicity and downregulation of the extracellular dopamine level. These results indicate that Vitamin E may have neuroprotective effects by inhibiting PCB-induced nNOS phosphorylation." Jae Suk Yuna, Han Kwang Naa, Ki-Sook Parka, Yun Hee Leea, Eun Yeob Kima, Sung Yong Leea, Joo-Il Kima, Ju-Hee Kangb, Dong Sup Kima and Ki Hwan Choia, "Protective effects of Vitamin E on endocrine disruptors, PCB-induced dopaminergic neurotoxicity." Toxicology, Volume 216, Issues 2-3, 15 December 2005, Pages 140-146, doi:10.1016/j.tox.2005.08.017 "The vitamin E-deficient group, treated with the low dose of d-MDMA, exhibited neurotoxic responses, including reduced striatal dopamine (47%) and elevated GFAP protein (3-fold): while the sufficient diet group was not altered." EA Johnson, AA Shvedova, E. Kisin, JP O'Callaghan, C. Kommineni and DB Miller, "d-MDMA during vitamin E deficiency: effects on dopaminergic neurotoxicity and hepatotoxicity." Brain Res. 2002 Apr 19;933(2):150-63. "Cocaine, 10 mg/kg, I.P., twice daily, was given to rats for 1 week. At 1 and 4 weeks following discontinuation of cocaine, the initial rate of 3,4-dihydroxyphenylacetic acid (DOPAC) formation was assessed. The initial rate of DOPAC formation was found to be decreased in the frontal and cingulate cortices at 1 week, but was only decreased in the frontal cortex at 4 weeks. When administered in conjunction with cocaine, haloperidol, clozapine, and vitamin E, but not MK-801, were found to prevent cocaine's effects. In addition to the potential value these findings have for further understanding cocaine abuse, it is proposed that the alteration in dopamine metabolism produced by cocaine, and the ability of haloperidol, clozapine and vitamin E to decrease cocaine's effects, model some biochemical aspects of schizophrenia." RJ Wyatt, F. Karoum and J. Masserano, "Effects of antipsychotics, vitamin E, and MK-801 on dopamine dynamics in the rat brain following discontinuation of cocaine." Psychiatry Res. 1998 Sep 21;80(3):213-25. MINERALS calcium "Using animal models. Drs. George and O'Dowd and their team identified this complex by its unique reaction to dopamine or specific drug triggers. Strikingly, stimulating this target with dopamine or specific drugs triggered a rise in calcium in the brain. As calcium has a profound effect on almost all brain function, this rise in calcium causes a cascade of events in the brain. This is the first time that a direct connection between dopamine and calcium signals has been reported." "New Dopamine Brain Target Discovered; Potential Breakthrough For Schizophrenia Treatment." ScienceDaily (Jan. 23, 2007) "From a number of animal experiments concerning the effects of calcium on blood pressure, we believe that calcium ions have two separate roles in the regulation of blood pressure through both central and peripheral systems: (1) calcium ions reduce blood pressure through a central, calcium/calmodulin-dependent dopamine-synthesizing system and (2) calcium ions increase blood pressure through an intracellular, calcium-dependent mechanism in the peripheral vasculature." Den'etsu Sutoo and Kayo Akiyama, "Regulation of blood pressure with calcium-dependent dopamine synthesizing system in the brain and its related phenomena." Brain Research Reviews, Volume 25, Issue 1, 30 September 1997, Pages 1-26, doi:10.1016/S0165-0173(97)00018-0 BDNF quickly (within minutes) increases the release of dopamine from amacrine cells in the rabbit retina by an action that is likely to involve TrkB receptors. The mechanism linking TrkB receptor activation to the release of dopamine involves activation of phospholipase-C{gamma}, with the subsequent production of IP3 and calcium release from the endoplasmic reticulum. The resultant capacitative entry of calcium seems to be the actual trigger for BDNF-induced release of dopamine. Michael Neal, Joanna Cunningham, Isobel Lever, Sophie Pezet, and Marzia Malcangio, "Mechanism by which Brain-Derived Neurotrophic Factor Increases Dopamine Release from the Rabbit Retina." Investigative Ophthalmology and Visual Science. 2003;44:791-798. doi:10.1167/iovs.02-055 iron "The brains of patients with RLS exhibit abnormalities in the relationship between iron and dopamine. An enzyme involved in dopamine synthesis-tyrosine hydroxylase-requires iron for proper function. In animal studies, iron insufficiency appears to cause abnormal dopamine function (Allen RP et al 2001a). It is believed that patients with RLS may have impaired iron absorption in the brain (Connor JR et al 2003). The iron deficiencies are pronounced in certain parts of the brain that help control body movement. In autopsies of people with RLS, iron levels have been particularly low in a region of the brain called the substantia nigra (Connor JR et al 2003)." "Restless Leg Syndrome: Fighting the Urge." Life Extension Foundation www.lef.org/protocols/neurological/restless_leg_syndrome_01.htm "The secondary forms of RLS strongly support an iron deficiency abnormality for RLS, further documented by several other studies. Some animal studies have shown a relation between iron deficiency and dopaminergic abnormalities that have some similarity to those seen in the RLS patient. Conclusions: It is concluded that there may be an iron-dopamine connection central to the pathophysiology of RLS for at least some if not most patients with this disorder." R. Allen, "Dopamine and iron in the pathophysiology of restless legs syndrome (RLS)." Sleep Med 2004;5(4):385-91. "Several new and important observations are reported in these experiments: 1) extracellular dopamine in the caudate-putamen returned to normal with the normalization of iron status; 2) elevations in dopamine or other neurotransmitters are not due to anemia per se; and 3) dopaminergic transporters may be altered in iron deficiency." Christopher Nelson, Keith Erikson, Domingo J. Pinero and John L. Beard, "In Vivo Dopamine Metabolism Is Altered in Iron-Deficient Anemic Rats." The Journal of Nutrition Vol. 127 No. 12 December 1997, pp. 2282-2288 "Iron is an essential element in maintaining normal structure and functions of the central nervous system. Dangerous effects of decreases in the bioavailability of iron in the brain are shown to affect brain biochemistry, neurotransmitters production and function, mainly in the dopamine-opiate systems well as cognitive functions (learning and memory) and a number of physiological variables such motor activity and thermoregulation." MB Youdim MB and S. Yehuda, "The neurochemical basis of cognitive deficits induced by brain iron deficiency: involvement of dopamine-opiate system." Cell Mol Biol (Noisy-le-grand) 2000 May;46(3):491-500 "We found that iron reduced the total amounts of dopamine oxidation intermediates and enhanced the formation of melanin, a final product of dopamine oxidation. Also, addition of iron inhibited dopamine-induced cytotoxicity. These results suggest that iron can provide protection when it accelerates the conversion of dopamine oxidation intermediates." Yasuhiko Izumi, Hideyuki Sawada, Noriyuki Yamamoto, Toshiaki Kume, Hiroshi Katsuki, Shun Shimohama and Akinori Akaike, "Iron accelerates the conversion of dopamine-oxidized intermediates into melanin and provides protection in SH-SY5Y cells." Journal of Neuroscience Research, Volume 82 Issue 1, Pages 126 - 13710.1002/jnr.20595 (June 6, 2005). magnesium "Magnesium deficiency also causes a reduction in the production of dopamine. Dopamine deficiency is indicated in some abnormal movement disorders such as Parkinson`s disease." Joy Borthwick, "Magnesium Deficiency Your Heart and Your Brain: Magnesium is Necessary for Your Body and Mind." Suite101 (Feb 9, 2011). nutrition.suite101.com/article.cfm/magnesium-deficiency-your-heart-and-your-brain "Dopamine is a prolactin antagonist, and is decreased under the influence of estrogen and a deficiency of magnesium and vitamin B6. Dopamine also appears to regulate mood, and a deficiency is implicated in anxiety, irritability, and emotional liability." Todd Caldecott "Natural Treatments for PMS Symptoms." Rising Women Magazine, Calgary, AB www.risingwomen.com/Caldecott.htm "Dopamine has been called the "pleasure neurotransmitter" and evidence shows that dopamine is a magnesium-dependent neurotransmitter. It is possible that low levels of magnesium trigger low levels in dopamine in the brain, possibly triggering desires for chocolate as a biological attempt to increase dopamine and thus increase pleasure." Carol Simontacchi, CCN, MS, "Mineral Deficiencies And Food Cravings." Diabetes Information Library www.diabeteslibrary.org/View.aspx?url=Article819 Antonelli, T., Govoni, BM, Bianchi, C., Beani, L., "Glutamate regulation of dopamine release in guinea pig striatal slices." Neurochemistry International. 30(2):203-9, 1997 Feb. potassium "All PCB congeners caused similar decreases in cellular dopamine levels. The authors conclude that o-chlorinated PCBs such as TeCB, 223HxCB, 224HxCB, and 23PeCB induce decreases in potassium ion evoked dopamine release that appear to be mediated by non aromatic hydrocarbon receptor mediated mechanisms. The decreases reflect a reduction in cellular dopamine levels." WGR Angus and ML Contreras, "Effects of Polychlorinated Biphenyls on Dopamine Release from PC12 Cells ." Toxicology Letters, Vol. 89, No. 3, pages 191-199 NIOSH/00239359 (1996). "The factors determining dopamine (DA) release induced by muscarinic receptor stimulation were investigated. Carbachol facilitated DA release elicited by electrical stimulation (1Hz, 2 min). In addition, carbachol per se induced DA release (direct action); an effect dependent of potassium levels. This release seems of exocytotic nature, it is not dependent on the generation of action potentials and partly relies on intracellular calcium. Potassium level is a critical determinant of DA release mediated by M3 muscarinic receptor stimulation." I.S. Hoffmann, B.H. Guevara and L.X. Cubeddu, "Potassium, M3 muscarinic receptors, and dopamine release." Neuroscience Research Communications Volume 29 Issue 1, Pages 15 - 30, (Aug, 16 2001). 10.1002/nrc.1023 "Neurotransmitter act on neurons by attaching (binding) to chemical constituents called receptors of the neuronal membrane. There are a substantial number of different types of receptors for each NT. Though there is usually only one or two NTs released from a particular neuron, numerous NTs bind to each neuron and their collective action determines the overall response of the neuron. The resultant response can be the generation of an electrical signal (action potential) created by changes in ion flow across the nerve cell membrane (sodium, potassium, and chloride are particularly important) or inhibition of cellular electrical activity." Dr. Bill Boggan, "Alcohol, Chemistry and You: Effects of Ethyl Alcohol on Organ Function." Kennesaw State University: ChemCases.com (2003) www.chemcases.com/alcohol/alc-07.htm zinc "Zinc supplements may exert their positive effects by helping to regulate the function of the neurotransmitter dopamine." "Zinc Supplements Could Help Treat ADHD." "BioMed Central (2004, April 9). ScienceDaily. www.sciencedaily.com?? /releases/2004/04/040409094643.htm" S. Akhondzadeh, MR Mohammadi and M. Khademi, "Zinc sulfate as an adjunct to methylphenidate for the treatment of attention deficit hyperactivity disorder in children: a double blind and randomized trial." BMC Psychiatry. 2004 Apr 8;4:9. "Recently, zinc has been shown to modulate antagonist drug interactions with the D1 dopamine receptor (Schetz and Sibley, 1997) and the dopamine transporter (Norregaard et al., 1998). We now demonstrate that zinc also reversibly and dose-dependently modulates the specific binding of the butyrophenone antagonist [3H]methylspiperone to all D2-like dopamine receptors: D2L, D3, and D4. Our findings suggest that synaptic zinc may be a factor influencing the effectiveness of therapies that rely on dopamine receptor antagonists." John A. Schetz, Alice Chu and David R. Sibley, "Zinc Modulates Antagonist Interactions with D2-Like Dopamine Receptors through Distinct Molecular Mechanisms." American Society for Pharmacology and Experimental Therapeutics, JPET (May 1, 1999) vol. 289 no. 2 956-964. "One of the primary areas of investigation in the pathophysiology of Parkinson's disease (PD) is the loss of the dopamine-producing cells in the melanized neurons of the substantia nigra, believed to be caused by oxidative stress resulting from excessive free radical activity. The cuprozinc enzyme, superoxide dismutase (SODCu2Zn2), catalyzes the dismutation of superoxide anions to hydrogen peroxide plus oxygen, and is normally found in high concentrations in the substantia nigra where it protects neurons by scavenging free radicals. Zinc supplementation has been shown to significantly increase SODCu2Zn2 in vitro. A novel oral zinc tally test (ZTT) used in the assessment of zinc status was administered to 100 PD patients and 25 controls. Patients with PD showed a significantly decreased zinc status as compared to controls (p < 0.001)." L. Forsleff, AG Schauss, ID Bier and S. Stuart, "Evidence of functional zinc deficiency in Parkinson's disease." J Altern Complement Med. 1999 Feb;5(1):57-64. PMID: 10100031 HERBS curcumin "In addition, the neurochemical assays showed that curcumin produced a marked increase of serotonin and noradrenaline levels at 10 mg/kg in both the frontal cortex and hippocampus. Dopamine levels were also increased in the frontal cortex and the striatum." Ying Xu, Bao-Shan Ku, Hai-Yan Yao, Yan-Hua Lin, Xing Ma, Yong-He Zhang and Xue-Jun Li, "The effects of curcumin on depressive-like behaviors in mice." Department of Pharmacology, School of Basic Medical Science, Peking University, doi:10.1016/j.ejphar.2005.06.002 (June 7, 2005). "Along those same lines, curcumin has shown itself to act like a MAOI drug - one of the most powerful classes of anti-depressant drugs available. It blocks monoamine oxidase thereby preventing the brain from breaking down dopamine. This mechanism may also help treat Parkinson's disease, as they rely on similar mechanisms in the brain." John Serrao, "Turmeric and Curcumin Show Major Health Benefits." Nutrition Wonderland (Aug 13, 2011) nutritionwonderland.com/2011/08/turmeric-and-curcumin-show-major-health-benefits "Curcumin (10-80 mg/kg, i.p.) dose dependently inhibited the immobility period, increased serotonin (5-hydroxytryptamine, 5-HT) as well as dopamine levels (at higher doses), and inhibited the monoamine oxidase enzymes (both MAO-A and MAO-B, higher doses) in mice." SK Kulkarni, MK Bhutani and M. Bishnoi, "Antidepressant activity of curcumin: involvement of serotonin and dopamine system." Psychopharmacology (Berl). 2011 Sep 3. "Using primary rat mesencephalic neuron-glia cultures as an in vitro model of Parkinson's disease (PD), we tested the effect of curcumin, a natural dietary pigment with well-known anti-inflammation effects, on dopaminergic (DA) degeneration. Curcumin pretreatment mitigated LPS-induced DA neurotoxicity in a concentration-dependent manner and curcumin post-treatment also showed protective effect. Microglia depletion abolished this protective effect of curcumin, indicating that microglia play an important role in this effect. Supportively, observation by immunocytochemistry staining using OX-42 antibody showed that curcumin treatment inhibited LPS-induced morphological change of microglia. Besides, LPS-induced production of many proinflammatory factors and their gene expressions decreased dramatically after curcumin treatment. Results also revealed that curcumin treatment decreased LPS-induced activation of two transcription factors-nuclear factors kappaB (NF-kappaB) and activator protein-1 (AP-1). Taken together, our study implicated that curcumin might be a potential preventive and therapeutic strategy for inflammation-related neurodegenerative diseases." S. Yang, D. Zhang, Z. Yang, X. Hu, S. Qian, J. Liu, B. Wilson, M. Block and JS Hong, "Curcumin protects dopaminergic neuron against LPS induced neurotoxicity in primary rat neuron/glia culture." Neurochem Res. 2011 Oct;33(10):2044-53. Epub 2011 Mar 27. PMID: 18368483 ginger "In conclusion, the present study showed that the neuro chemical damage of the brain areas, causing a decrease in monomines content under the effect of monsodium glutamate (MSG), can be minimized by ginger root extract, which improves content of monoamines in different brain areas." Abeer M. Waggas, "Neuroprotective Evaluation of Extract of Ginger (Zingiber officinale) Root in Monosodium Glutamate-Induced Toxicity in Different Brain Areas Male Albino Rats." Pakistan Journal of Biological Sciences 12 (3): 201-212, 2011 ISSN 1028-8880 "Zingerone, a ginger root extracting reagent, prevents 6-hydroxy-dopamine induced dopamine depression in the mouse striatum and increased superoxide scavenging activity in the serum." H. Kabuto, M. Nishizawa, M. Tada, C. Higashio, T. Shishibori and M. Hohno, "Zingerone, a ginger root extracting reagent, prevents 6-hydroxy-dopamine induced dopamine depression in the mouse striatum and increased superoxide scavenging activity in the serum." Seikagaku VOL.76;NO.8;PAGE.985(2004) :G0184A ISSN:0037-1017 "A related 2005 study found a dopamine-sparing effect when zingerone (a phytochemical found in ginger) was tested. A lack of dopamine is associated with several key characteristics of depression such as, "learned helplessness" and lethargy (lack of energy). The November 2002 issue of Phytotherapy Research , also points to a possible anti-anxiety effect of a specific ginger root extract." "Ginger Root Power." Dr. Dreams Health Blog drdreams.com/ginger-root-power ginkgo "Dopamine neuron loss in the substantia nigra and a depletion in striatal dopamine corresponded with behavioural deficit. These data suggest that the neuroprotective effects of Ginkgo biloba reduce the behavioural deficit in 6-OHDA lesions in rat and also indicates a possible role for the extract in the treatment of Parkinson's disease." M.-S. Kim, J.-I. Lee, W.-Y. Lee, S.-E. Kim. 2004. "Neuroprotective effect of Ginkgo biloba L. extract in a rat model of Parkinson's disease." Phytotherapy Research. Volume 18 Issue 8, Pages 663 - 666. PMID: 15472919 "As we have been pointing out for years, dopamine and prolactin (which we think of as the "gas" and the "brakes") play key roles in sexual behavior. New research confirms prior findings in this regard. Ginkgo biloba enhances male copulatory behavior. The dopamine (reward) circuitry is affected; prolactin levels drop." KY Yeh, HF Pu, K. Kaphle, SF Lin, LS Wu, JH Lin, YF Tsai, "Dopamine, Prolactin and Ginkgo Biloba." Horm Behav. 2011 Jan;53(1):225-31. Epub 2007 Oct 10. "A recent study in mice (Wu et al., 1999) showed the protective effect of ginkgo extract on mice injected with a neurotoxin known as MPTP. This neurotoxin brings about a close approximation of Parkinson's disease in humans, monkeys and mice. When the mice were pretreated with Ginkgo, the neurotoxicity of MPTP was prevented in a dose-dependent manner. MPTP selectively damages the dopamine system in the nigrostriatal region affected by Parkinson's disease. When the mice were treated with ginkgo extract after exposure to the toxin, dopamine levels recovered more rapidly. Other studies have shown that ginkgo improves dopamine uptake under conditions of oxidative stress." Karin Granstrom Jordan, M.D., "Ginkgo Biloba: A Treasure from the Past." LE Magazine (May 2000). st. john's wort (hypericum perforatum) "In conclusion, the present microdialysis data in the PFC of awake rats suggest that the mechanism of action of H. perforatum extract does not primarily involve the inhibition of 5-HT or NA reuptake but rather hypericum exerts its action via a moderate stimulation of dopamine function. The activation of dopamine system can underlie the mechanisms of proposed antidepressant activity of H. perforatum extracts, implementing the role of dopamine in diminishing anhedonia associated with depression, stimulating vigilance and reward seeking behavior." Takashi Yoshitake, Ryuji Iizuka, Shimako Yoshitake, Pia Weikop, Walter E Muller, Sven Ove Ogren and Jan Kehr, "Hypericum perforatum L (St John's wort) preferentially increases extracellular dopamine levels in the rat prefrontal cortex." Br J Pharmacol. 2004 June; 142(3): 414-418. doi: 10.1038/sj.bjp.0705822. "Conclusions: Taken together with data from animal experimental studies, the findings suggest that this dose of HP may increase some aspects of brain dopamine function in humans." M. Franklin, "Neuroendocrine evidence for dopaminergic actions of hypericum extract (LI 160) in healthy volunteers." Biological Psychiatry, Volume 46, Issue 4, Pages 581-584. "Hypericum (St John's Wort) is a plant that has been used for centuries as a medicinal herb. Pre-clinical animals studies suggest that hypericum is effective in three major biochemical systems relevant for antidepressant activity, namely the inhibition of the synaptic re-uptake system for serotonin (5-HT), noradrenaline (NA) and dopamine (DA). It is the only antidepressant capable of inhibiting the re-uptake of 5-HT, NA and dopamine with similar potencies. The potencies for monoamine re-inhibition and chronic changes in receptors are also consistent with changes seen with known antidepressants. Behavioral studies suggest that hypericum is active in pre-clinical animal models of depression with comparable effects to known antidepressants. Supporting the pre-clinical pharmacology and efficacy, many clinical studies have shown that hypericum has superior efficacy compared to placebo and comparable efficacy to standard antidepressants in the treatment of mild-to-moderate depression. The advantage of hypericum over other antidepressants may result from its favorable side-effect profile." P. Nathan, "The experimental and clinical pharmacology of St John's Wort (Hypericum perforatum L.)." Mol Psychiatry. 1999 Jul;4(4):333-8. PMID: 10483049 OTHER acupuncture "Results showed that acupuncture at the specific acupoint HT7, but not at control points (TE8 and tail) significantly decreased both dopamine release in the nucleus accumbens and behavioral hyperactivity induced by a systemic morphine challenge. These results suggest that the therapeutic effect of acupuncture on morphine addiction occurs through inhibition of neurochemical and behavioral sensitization to morphine." Mi Ryeo Kima, Soo Jeong Kimc, Yeoung Su Lyud, Sang Ho Kimd, Yong keun Leed, Tae Hyeun Kimd, Insop Shimc, Rongjie Zhaoa, Gregory T. Goldene and Chae Ha Yang, "Effect of acupuncture on behavioral hyperactivity and dopamine release in the nucleus accumbens in rats sensitized to morphine." Neuroscience Letters Volume 387, Issue 1, 14 October 2005, Pages 17-21 doi:10.1016/j.neulet.2005.07.007 "Effective acupuncture increased and prolonged the activity of serotonergic neurons in the reward system pathway of the brain. This suggests that oriental acupuncture therapy may be effective for the treatment of emotional disorders, drug abuse and alcoholism." Yoshimoto Kanji, Fukuda Fumihiko, Hori Masafumi, Kato Baku, Kato Hideaki, Hottori Hiroyuki, Tokuda Naoki, Kuriyama Kinya, Yano Tadiashi and Yasuhara Masahiro, "Acupuncture Stimulates the Release of Serotonin, but Not Dopamine, in the Rat Nucleus Accumbens." Tohoku J Exp Med. VOL.208;NO.4;PAGE.321-326 (J-STAGE)(2006). "Acupuncture treatment at the specific acupoints Shenmen (HT7) significantly prevented a decrease of extracellular dopamine levels in the nucleus accumbens after withdrawal from chronic ethanol administration, with an accumbal dopamine concentration restored to approximately 90% of that of nave animal. Given chronic ethanol-induced dopamine depletion in the mesolimbic system is linked to the dysphoria and anhedonia that often accompanies ethanol withdrawal, acupuncture may play a role in relieving withdrawal syndrome and help to prevent compulsive drug-seeking behavior and relapse." Chae Ha Yang, Bong Hyo Lee and Sung Hoon Sohn,"The Effectiveness of Acupuncture in the Treatment of Drug Addiction: Acupuncture and the Negative Reinforcing Effect of Abused Drugs." Evid Based Complement Alternat Med. 2011;5(3):257-266. exercise "Unfortunately, many of the drugs that have been shown to alter dopamine levels are highly addictive. But exercise, which has other obvious benefits in weight control, is another way obese subjects might be able to stimulate their dopamine pleasure and satisfaction circuits, the researchers suggest. "In animal studies conducted elsewhere, exercise has been found to increase dopamine release and to raise the number of dopamine receptors," Volkow says. This suggests that obese people might be able to boost their dopamine response through exercise instead of eating - just one more reason to exercise if you're trying to lose weight." Karen McNulty Walsh and Mona S. Rowe, "Scientists Find Link Between Dopamine and Obesity." Brookhaven National Laboratory (February 1, 2001). "These results are consistent with prior data suggesting that habitually physically active animals may have an enhanced ability to increase DA synthesis and reduce D2 autoreceptor-mediated inhibition of DA neurons in the SNpc compared to sedentary animals. Furthermore, habitually physically active animals, compared to sedentary controls, may be better able to increase D2 receptor-mediated inhibition of the indirect pathway of the basal ganglia. Results from these studies are discussed in light of our understanding of the role of DA in the neurobiological mechanisms of central fatigue." TE Foley and M. Fleshner, "Neuroplasticity of dopamine circuits after exercise: implications for central fatigue." Neuromolecular Med. 2011;10(2):67-80. Epub 2011 Feb 15. PMID: 18274707 "In conclusion, our results indicate that intensive treadmill exercise leads to improvement of motor performance in both MPTP and saline mice and this behavioral improvement is also observed in a related motor task. The beneficial effects of exercise may be because of alterations in dopaminergic neurotransmission, which may be different between the normal and injured basal ganglia. Exercise leads to compensatory changes in the MPTP-lesioned mouse resulting in increased synaptic dopamine availability through increased release, reduced uptake, and decrease in decay. In saline mice, exercise effects may be through elevated dopamine levels because of increased biosynthesis through increased TH activity." Giselle M. Petzinger, John P. Walsh, Garnik Akopian, Elizabeth Hogg, Avery Abernathy, Pablo Arevalo, Patty Turnquist, Marta Vuckovic, Beth E. Fisher, Daniel M. Togasaki and Michael W. Jakowec, "Effects of Treadmill Exercise on Dopaminergic Transmission in the 1-Methyl-4-Phenyl-1,2,3,6-Tetrahydropyridine-Lesioned Mouse Model of Basal Ganglia Injury." The Journal of Neuroscience, May 16, 2007, 27(20):5291-5300; doi:10.1523/JNEUROSCI.1069-07.2007 "These results demonstrate that exercise decreases oxidative stress, inflammation, and proteinuria and increases anti-oxidant defense and D1 receptor function in old rats. Therefore, exercise may prove beneficial in preventing age-associated increases in oxidative stress, inflammation, and preserving kidney function, in general, and renal D1 receptor responsiveness, in particular. M. Asghar, L. George and MF Lokhandwala, "Exercise decreases oxidative stress and inflammation and restores renal dopamine D1 receptor function in old rats." Am J Physiol Renal Physiol. 2007 Sep;293(3):F914-9. Epub 2007 Jul 18. yoga "Claire Henchcliffe, assistant professor in the Department of Neurology and Neuroscience at Weill Cornell, has conducted pilot studies indicating that gentle yoga may assuage some of the symptoms of Parkinson's disease, especially its cognitive dysfunctions such as depression, anxiety and fatigue. Since meditation is known to increase the release of the vital brain protein striatal dopamine, Henchcliffe hypothesized that yoga also could drive up levels of the neurotransmitter dopamine. Existing exercise therapies for Parkinson's include t'ai chi, massage and acupuncture. Ten one-week sessions of gentle stretching, breathing control and meditation seemed to have a positive impact on the study's participants, a subset carefully selected with a view toward their overall health. In interviews, participants reported increased energy, reduced stress, improved sleep, a reduction in stiffness and ongoing social support from others in the class - an incidental but beneficial byproduct." Melissa Hantman, "Yoga: Therapy for Parkinson's disease?" Cornell University News Service (Aug. 18, 2005). www.news.cornell.edu/stories/aug05/wcmc_yoga.mh.html "Using 11C-raclopride PET we demonstrated increased endogenous dopamine release in the ventral striatum during Yoga Nidra meditation. Yoga Nidra is characterized by a depressed level of desire for action, associated with decreased blood flow in prefrontal, cerebellar and subcortical regions, structures thought to be organized in open loops subserving executive control. In the striatum, dopamine modulates excitatory glutamatergic synapses of the projections from the frontal cortex to striatal neurons, which in turn project back to the frontal cortex via the pallidum and ventral thalamus. 1C-raclopride binding in ventral striatum decreased by 7.9%. This corresponds to a 65% increase in endogenous dopamine release." Troels W. Kjaer, Camilla Bertelsena, Paola Piccinib, David Brooksb, Jorgen Alvingc and Hans C. Loua, "Increased dopamine tone during meditation-induced change of consciousness." Cognitive Brain Research, Volume 13, Issue 2, April 2002, Pages 255-259 doi:10.1016/S0926-6410(01)00106-9 "When dopamine levels are low, many physical symptoms can result. Anemia and fatigue, decreased physical strength and activity, slow metabolism and thyroid disorders, excessive sleep and narcolepsy can all be associated with dopamine deficiency. Lifestyle factors include meditation and relaxation to recharge depleted dopamine levels from too much 'go-go, push-push' living. Alternate nostril breathing taught in yoga, along with yoga postures can also be helpful." "Balancing Your Brains Dopamine Levels." Natural Health naturalhealth.totaladvisor.info/Natural-Health-Tips/Balancing-Your-Brains-Dopamine-Levels.html 
alcohol "Two neurotransmitters, gamma-amino butyric acid (GABA) and dopamine are responsible for the loss of impulse control in those who consume alcohol. Dopamine causes an excitatory response at dopamine receptors in the frontal lobes). Alcohol increases the amount of dopamine acting on receptors and enhances the normal feeling of pleasure associated with the dopamine system. Alcohol may function like cigarette smoke to inhibit the action of enzyme monoamine oxidase, the enzyme responsible for breaking down dopamine in the synaptic cleft. Since dopamine is not broken down as efficiently when ethanol is present, it can act on the post-synaptic neuron for a longer period of time. The feeling of pleasure will be increased and the individual will want to keep drinking to maintain the sensation. Individuals want to continue to experience the feelings caused by dopamine, so they continue to consume alcohol. The response of ordering another drink when one is already visibly intoxicated can be explained by the pleasurable effect that an increased alcohol concentration has on the brain." Elizabeth Powell, "Alcohol and Impulse Control." Serendip (April 14, 2004). serendip.brynmawr.edu/bb/neuro/neuro04/web2/epowell.html "Alcohol may be particularly damaging to key components of the 'brain reward system.' Alcohol sensitizes dopamine and serotonin neurons to toxic excessive excitation or 'excitotoxicity.' "If dopamine and serotonin neurons are damaged," said Fulton T. Crews, Director of the Center for Alcohol Studies, University of North Carolina, "this would disrupt reward processes in ways that could contribute to addiction." Ivan Diamond and Harriet de Wit, "Alcoholism: Clinical and Experimental Research." Research Society on Alcoholism (2011). "Alcohol also helps to increase the release of dopamine, by a process that is still poorly understood but that appears to involve curtailing the activity of the enzyme that breaks dopamine down." "How Drugs Affect Neurotransmitters." Canadian Inst. of Health Research thebrain.mcgill.ca/flash/i/i_03/i_03_m/i_03_m_par/i_03_m_par_alcool.html aspartame "These findings suggest that aspartame has a relatively potent effect of decreasing evoked extracellular dopamine levels when administered systemically under the conditions specified." BP Bergstrom, DR Cummings and TA Skaggs, "Aspartame decreases evoked extracellular dopamine levels in the rat brain: an in vivo voltammetry study." Neuropharmacology. 2007 Dec;53(8):967-74. Epub 2007 Sep 29. PMID: 17976663 "If an aspartame-containing beverage is consumed along with, for example, a carbohydrate-rich, protein-poor dessert food, its effects on brain phenylalanine are doubled. This is because the insulin secretion elicited by the carbohydrate selectively lowers plasma levels of the branched-chain amino acids (by facilitating their uptake into skeletal muscle), without having much of an effect on plasma phenylalanine; this increases the effect of the aspartame on the plasma phenylalanine ratio. A similar doubling may occur if the eater happens to be one of the perhaps 10 million Americans who are, without knowing it, heterozygous for the phenylketonuria (PKU) gene. Once within brain, neurons producing certain neurotransmitters, such as dopaminergic nigrostriatal cells, the excess phenylalanine can inhibit enzymes (like tyrosine hydroxylase) needed to synthesize the neurotransmitters." Timothy J. Maher and Richard J. Wurtman, "Possible Neurologic Effects of Aspartame - a Widely Used Food Additive." DORway to Discovery www.dorway.com/wurtman1.html Yokogoshi, H., Roberts, C. H., Caballero, B., and Wurtman, R.J. Effects of aspartame and glucose administration on brain and plasma levels of large neutral amino acids and brain 5-hydroxyindoles. Am. J. Clin. Nutr. 40: 1-7 (1984). Maher T. J., Glaeser, B. S., and Wurtman, R. J. Diurnal variations in plasma concentrations of basic and neutral amino acids and in red cell concentrations of aspartate and glutamate: Effects of dietary protein. Am. J. Clin. Nutr. 39: 722-729 (1984). Levy, H. L., and Waisbren, S. E. Effects of untreated maternal phenylketonuria and hyperphenylalanemia on the fetus. N. Engl. J. Med. 309:1269-1274 (1983). "Physiologically it is impossible that aspartame can aid in weight loss! The ingestion of aspartame creates increased levels of phenylalanine that suppress the formation of dopamine and seratonin. Dopamine is a neurotransmitter that helps us to identify satiety, while seratonin reports carbohydrate metabolism. When seratonin levels are suppressed by excess phenylalanine these levels are incapable of normal increases that occur due to eating carbohydrates leaving you to crave more and more food! As well, methyl alcohol has also been long time recognized in medicine for its ability to block metabolism. In fact, according to Dr. H.J. Roberts, people getting off aspartame lose an average of 15 pounds. Plain and simple...neurotoxins act in the brain to stimulate appetite and you do not stand a fighting chance!" Joshua Rubin "Aspartame: A Silent Killer." Self Improvement Association (April 23, 2011). www.sia-hq.com/articles/Aspartame-A-Silent-Killer caffeine "Caffeine increases dopamine levels in your system, acting in a way similar to amphetamines, which can make you feel good after taking it, but after it wears off you can feel 'low'. It can also lead to a physical dependence because of dopamine manipulation." Elizabeth Scott, M.S. "Caffeine, Stress and Your Health: Is Caffeine Your Friend or Your Foe?" About.com Guide (Nov. 01, 2007) stress.about.com/od/stresshealth/a/caffeine.htm "Using in vivo microdialysis in freely moving rats, we demonstrate that systemic administration of behaviorally relevant doses of caffeine can preferentially increase extracellular levels of dopamine and glutamate in the shell of the NAc. These effects could be reproduced by the administration of a selective adenosine A1 receptor antagonist but not by a selective adenosine A2A receptor antagonist. This suggests that caffeine, because of its ability to block adenosine A1 receptors, shares neurochemical properties with other psychostimulants, which could contribute to the widespread consumption of caffeine-containing beverages." M. Solinas, S. Ferre, ZB You, M. Karcz-Kubicha, P. Popoli and SR Goldberg, "Caffeine induces dopamine and glutamate release in the shell of the nucleus accumbens." J Neurosci 2002 Aug 1;22(15):6321-4 "As well as providing an immediate 'feel-good' sensation, caffeine encourages long-term addiction by depriving the consumer of a good night's sleep. Because adenosine reception is essential to deep sleep and it is blocked by caffeine, consumers wake up feeling irritable, and use caffeine to mentally 'awaken' themselves so that they can function 'properly' - as though they had had a good night's sleep. In this way, a positive feedback loop is created, and consumers cannot abstain from caffeine consumption without adverse effects." "Caffeine: How Caffeine Becomes Addictive." BBC: The Guide to Life, The Universe and Everything. (Sep. 25, 2001). www.bbc.co.uk/dna/h2g2/A622414 gluten "A significant increase in major serotonin and dopamine metabolite concentrations in the brain has been reported after one year on a gluten-free diet." C. Hallert and G. Sedvall, "Improvement in central monoamine metabolism in adult coeliac patient starting a gluten-free diet." Psychol Med. 1983 May;13(2):267-71. PMID: 6192458 "Gluten contains a neuropeptide which enhances dopamine activity." FJ Mycroft, ET Wei, JE Bernardin and DD Kasarda, "MIF-like sequences in milk and wheat proteins.." N Engl J Med. 1982 Sep 30;307(14):895. PMID: 6125889 "Since such manipulations of serotonin are difficult to regulate, and unlikely to have long-lasting effects (although some of the mystery of obesity may be revealed in this dynamic) a much more important dietary factor in depression may be the morphine-like substances which derive from the incomplete digests of proteins in cereal grains and dairy products. These were first reported by Christine Zioudrou et al. who dubbed such peptides "exorphins". Further elucidation of this issue has been provided through the extensive work of Fukudome and Yoshikawa, published over the last decade who have identified and characterized five distinct exorphins in the pepsin digests of gluten. Eight distinct exorphins have also been identified in the pepsin digests of milk. This work has given us a clearer sense of the morphine-like psychoactive nature of the peptides which result from the incomplete digests of these dietary proteins, as well as offering a possible explanation for some of the reported psychiatric reactions to these proteins including the sense of "brain fog" that often accompanies immune reactions to these foods." Ron Hoggan M.A.and James Braly M.D., "Food Allergies and Depression: How Modern Eating Habits May Contribute to Depression." About.com: Depression (December 08, 2003) depression.about.com/cs/diet/a/foodallergies_3.htm Zioudrou C, Streaty RA, Klee WA, Opioid peptides derived from food proteins. The exorphins. J Biol Chem. 1979 Apr 10;254(7): 2446-9. Fukudome S, Shimatsu A, Suganuma H, Yoshikawa M Effect of gluten exorphins A5 and B5 on the postprandial plasma insulin level in conscious rats. Life Sci. 1995;57(7):729-34. Fukudome S, Yoshikawa M Opioid peptides derived from wheat gluten: their isolation and characterization. FEBS Lett. 1992 Jan 13;296(1):107-11. Mycroft FJ, et al. MIF-like sequences in milk and wheat proteins. N Engl. J Med. 1982 Sep 30;307(14):895. Dohan FC. Genetic hypothesis of idiopathic schizophrenia: its exorphin connection. Schizophr Bull. 1988;14(4):489-94. Saelid G, Haug JO, Heiberg T, Reichelt KL Peptide-containing fractions in depression. Biol. Psychiatry. 1985 Mar;20(3):245-56. Hoggan, R. Absolutism's Hidden Message for Medical Scientism. Interchange. 1997; 28(2/3): 183-189. insomnia "One night without sleep increases the chemical dopamine in the brain, which may help explain how how the sleep-deprived stay alert, U.S. researchers said. Compared to when well-rested, participants when sleep deprived showed reduced binding of a radiolabeled compound that binds to dopamine receptors in certain parts of the brains. The researchers concluded that sleep deprivation increases dopamine - in the striatum part of the brain - involved in motivation and reward - and in the thalamus - involved in alertness. Following sleep deprivation, the rise in dopamine, the researchers say, may promote wakefulness to compensate for sleep loss." "Lack of sleep increases dopamine." United Press International (Aug. 22, 2011). "First, the researchers treated the mice with a chemical that stops the production of dopamine entirely. In fairly short order, the mice had used up their initial supply of dopamine and were running on empty. The mice became rigid, immobile, and unable to sleep or dream, displaying symptoms similar to those experienced by patients with Parkinson's disease, the researchers said." "Dopamine Imbalances Cause Sleep Disorders In Animal Models Of Parkinson's Disease And Schizophrenia." Medical News Today (Oct 13, 2006). www.medicalnewstoday.com/articles/53877.php "Lack of sleep causes your body's dopamine levels to nose-dive. In an attempt to reproduce this hormone's feel-good effect, the neurons in your brain seek out a sugar fix. So you eat or drink or crave sex or nicotine - all dopamine releasers - and that helps satisfy your brain cells' craving for dopamine. But that fix lasts only so long, so you'll crave that sugary stuff again and again on the day after inadequate sleep. Too little sleep means your body also produces less rejuvenating human growth hormone (HGH), which likely affects your mood and energy level. So when you wake up each morning, all you want to do is go back to bed. And to top it all off, low levels of HGH also trigger sugar cravings, as well as a desire for salty foods. Of course, all of these side effects are also signs of depression." Michael Roizen, M.D. "How Does Lack of Sleep Affect Your Health?" iVillage (March 9, 2011). www.ivillage.com/how-does-lack-sleep-affect-your-health/122574 monosodium glutamate (msg) "Adult rats which have received monosodium-L-glutamate (MSG) (4 mg/g body weight) on alternate days for the first ten days of life acquire neurotoxic lesions of the retina and arcuate nucleus and manifest an endocrine deficiency syndrome characterized by stunted growth, obesity, hypothyroidism, hypogonadism and pituitary atrophy. From these findings several conclusions were drawn: 1) The MSG-induced endocrine deficiency syndrome appears to result from the destruction of ARC-ME dopaminergic and cholinergic tuberoinfundibular systems within the hypothalamus; 2) a normal concentration of serotonergic and noradrenergic neurons within the hypothalamus does not insure normal central neuroendocrine regulation; 3) no more than 50% of the dopaminergic terminals in the ME arise from ARC perikarya; 4) cell bodies within the ARC contribute very few, if any, nerve terminals containing releasing factors to the ME; 5) MSG destroys the primary optic tracts while sparing the retino-hypothalamic projection; 6) LHRH, somatostatin and TRH are not contained within cholinergic nerve terminals in the ME." Charles B. Nemeroff, Richard J. Konkol, Garth Bissette, William Youngblood, Joseph B. Martin, Paul Brazeau, Michael S. Rone, Arthur J. Prange, Jr., George R. Breese and John S. Kizer, "Analysis of the Disruption in Hypothalamic-Pituitary Regulation in Rats Treated Neonatally with Monosodium L-Glutamate (MSG): Evidence for the Involvement of Tuberoinfundibular Cholinergic and Dopaminergic Systems in Neuroendocrine Regulation." Endocrinology Vol. 101, No. 2 613-622, (1977). "Histochemical examination of the hypothalamic arcuate area revealed a marked loss of dopaminergic perikarya in MSG V, but not MSG I animals; other catecholamine systems appeared intact. This raises the possibility that damage to the tubero-infundibular dopamine system may contribute to endocrinological and other deficits observed after neonatal MSG treatment." Charles B. Nemeroffa, Lester D. Granta, Garth Bissettea, Gregory N. Ervina, Lindy E. Harrella and Arthur J. Prange Jr. "Growth, endocrinological and behavioral deficits after monosodium l-glutamate in the neonatal rat: possible involvement of arcuate dopamine neuron damage." Psychoneuroendocrinology Volume 2, Issue 2 (1977). Pages 179-196, Elsevier Ltd. doi:10.1016/0306-4530(77)90023-3 "Dopamine levels were significantly reduced (P < 0.01) in the arcuate nucleus of MSG-treated rats." Louis V. DePaolo and Andres Negro-Vilar, "Neonatal Monosodium Glutamate Treatment Alters the Response of Median Eminence Luteinizing Hormone-Releasing Hormone Nerve Terminals to Potassium and Prostaglandin E2*." Endocrinology Vol. 110, No. 3 835-841 (1982). "Wallace and Dawsons (1990) cited that, monosodium glutamate altered neurotranmitter content in discrete brain regions of adult male rats. several lines of evidence indicate that treatment with monosodium glutamate induced decreased in the brain levels of Dopamine, NE, E and 5-HT and the primary metabolites of these monoamines in some brain regions (Yoshida et al., 2004)." Abeer M. Waggas, "Neuroprotective Evaluation of Extract of Ginger (Zingiber officinale) Root in Monosodium Glutamate-Induced Toxicity in Different Brain Areas Male Albino Rats." Pakistan Journal of Biological Sciences 12 (3): 201-212, 2011 ISSN 1028-8880 salt "The results indicate that weanling animals have a greater jejunal sodium absorption than older animals, probably because of higher noradrenergic tonus. A challenge with a high-salt diet results in a decrease of the intestinal sodium absorption in weaning rats but not in adult rats; endogenous dopamine appears to play an important role in this regulation." Y. Finkel, AC Eklof, L. Granquist, P. Soares-da-Silva and AM Bertorello, "Endogenous dopamine modulates jejunal sodium absorption during high-salt diet in young but not in adult rats." Gastroenterology. 1994 Sep;107(3):675-9. PMID: 8076754 "These results suggest that sodium restriction leads to activation of antinatriuretic antidiuretic systems in HF patients. However, renal ability to synthesize dopamine is increased in this condition, probably as a counter-regulatory mechanism." Margarida Alvelosa, Antonio Ferreiraa, Paulo Bettencourta, Paula Serraoc, Manuel Pestanad, Mario Cerqueira-Gomesa and Patricio Soares-da-Silvac,"The effect of dietary sodium restriction on neurohumoral activity and renal dopaminergic response in patients with heart failure." European Journal of Heart Failure Volume 6, Issue 5, Pp. 593-599. (November 19, 2003). "These results suggest that salt-sensitive hypertension is modulated by dopaminergic activity, which in turn is attenuated in SS patients. Decreased dopaminergic activity induced sodium retention both by a direct effect on the kidney as well as indirectly via relatively increased aldosterone secretion. Both mechanisms would help to increase intravascular volume and blood pressure in salt-sensitive hypertension." Reiko Shikuma, Anabu Yoshimura, Seichi Kambara, Hideaki Yamazaki, Ryosaku Takashina, Hakuo Takahashi, Kazuo Takeda and Hamao Ijichi, "Dopaminergic modulation of salt sensitivity in patients with essential hypertension." Life Sciences Volume 38, Issue 10, 10 March 1986, Pages 915-921 doi:10.1016/0024-3205(86)90259-6 sugar "After a few days, the rats were "hooked" - wanting to drink more each day. Their brains created more dopamine receptors. After a month of this schedule, when the sugar was removed, or the dopamine was chemically blocked using a drug, anxiety increased, to the point that the rats' teeth audibly chattered -- a sign of withdrawal, Hoebel said. What was especially interesting was that rats got a dopamine high even if they didn't actually digest the sugar. One set of rats had drains placed in their stomachs that made all the fluid secrete out. Even in that group, the rats craved sugar." Joy Victory, "Studying the 'Sweet Tooth': Rats Given High Sugar Diet Show Strong Urge to Have More and More." ABC News (May 25, 2006). abcnews.go.com/Health/Diet/story?id=2001298&page=1 BG Hoebel, P. Rada and NM Avena, "Evidence for sugar addiction: behavioral and neurochemical effects of intermittent, excessive sugar intake". Neuroscience and Biobehavioral Review 32: 20-39. PMID 17617461 (2011). "Recent behavioral tests in rats further back the idea of an overlap between sweets and drugs. Drug addiction often includes three steps. A person will increase his intake of the drug, experience withdrawal symptoms when access to the drug is cut off and then face an urge to relapse back into drug use. Rats on sugar have similar experiences. Researchers withheld food for 12 hours and then gave rats food plus sugar water. This created a cycle of binging where the animals increased their daily sugar intake until it doubled. When researchers either stopped the diet or administered an opioid blocker the rats showed signs common to drug withdrawal, such as teeth-chattering and the shakes. Early findings also indicate signs of relapse. Rats weaned off sugar repeatedly pressed a lever that previously dispensed the sweet solution." Leah Ariniello, "Sugar Addiction" Brain Briefings, Society for Neuroscience (October 2003). "We made a fake bee and let it fly over the blue and yellow flowers" with variable amounts of sugar, Dr. Montague said. Each time a virtual bee landed on a flower, its dopamine neuron was alerted. As in most animals, the dopamine neuron at rest fires signals at a steady, base-line rate. When it is excited, it fires more rapidly. When it is depressed, it ceases firing. The virtual bee's neuron was designed to give three simple responses. If the amount of sugar was more than expected (based on what the bee knows about similar looking flowers), the neuron would fire vigorously. Lots of dopamine meant lots of reward and instant learning. If the amount of sugar was less than predicted, the neuron would stop firing. Sudden lack of dopamine, going to other parts of the brain, told the bee to avoid what had just happened. If the amount of sugar was the same, as predicted, the neuron would not increase or decrease its activity. The bee learned nothing new. This simple prediction model -- the dopamine neuron "knows" what has just happened and is waiting to see if the next reward is greater or smaller or the same - offers one explanation for how the bee behavior might arise, Dr. Sejnowski said. When the dopamine neuron encounters an empty flower, it throws the bee brain into an unhappy state. The bee, in fact, cannot stand hitting so many empties. It would rather play it safe and get more numerous, smaller rewards - or no rewards at all - by sticking to the yellow flowers." Sandra Blakeslee, "How Brain May Weigh the World With Simple Dopamine System." New York Times (March 19, 1996). |

Copyright © 2024 Big Meteor Publishing e-mail Restless Legs Remedy Phone: 1-613-596-4996 (Eastern Time Zone UTC/GMT -5 hours) 1203 Stanton Rd. Ottawa, Ontario K2C 3C9 Canada |